OK, a bullet to the head would generally do it, but what if you’ve lovingly created a character and now want to kill them off a little less dramatically. A little more slowly perhaps?
Death is around us all the time, but it’s not something we think about and rarely witness. If we do get a chance to say a last goodbye to someone dear to us we certainly don’t take notes for future reference. So what does death and the dying look like? What is the process, what happens and how do doctors make a dying diagnosis?
This is a big subject, but hopefully, as a writer, you will find all you need to kill with confidence (literary speaking)
Fact : 0nly 10% of deaths are sudden
What’s the Prognosis Doc?
For the most, death is a long drawn out process shrouded in mystery and contradiction. The medical profession (in the UK at least) don’t have a single definitive way of diagnosing the terminal decline of a chronically ill patient, or how long it will take them to die. Even the Harley Street Consultant with his £200 an hour smile and Italian leather shoes relies on acquired knowledge, the surmised results of medical surveys and past experience.
Of course there are circumstances where imminent death is inevitable. A person with their arm trapped under a boulder, who makes the decision to self-amputate with a pocket knife, is certain to die. That has to be a given. . . Wait a mo. Didn’t he write a book, and wasn’t there a film too?
The wonderful thing about the human condition is that we take the greatest pleasure in defying expectation.
The truth is doctors too are stuck between a rock and a hard place. If they make a gloomy prognosis, treatment may be stopped and cancel out a percentage chance of survival. On the other hand an optimistic prognosis could mean a patient not getting end of life care and a dignified death.

“Medical staff worry about mistiming a dying diagnosis”
Generally speaking, if it is thought death might happen within a few weeks, then invasive medical treatments will be stopped if the distress they cause outweighs any positive results. Your character will be granted time to put his affairs in order and put steps in place for a ‘good’ death.
However, studies show that, in many cases invasive and futile medical treatments are continued right up the last phases of life, even when a patient is diagnosed as dying. Only in the case of cancer, do doctors generally feel comfortable transferring patients into Palliative Care. For other life limiting conditions, such as heart failure, doctors are likely to delay a dying diagnosis and admit patients to hospitals for medical treatment. In hospices and hospital, medical staff worry about mistiming a dying diagnosis and distressing patients and their families. In nursing homes, the study found that staff may not have the skills to recognise a resident is dying or give end of life care.
Doctors and nurses are human just like the rest of us.
The Physiology of Death
There are symptoms that indicate a patient is dying. Laboratory blood tests can assess the condition of plasma, white blood cells and the immune system, but for the most the medical profession rely on Hippocratic Observation; feeling, looking and listening for physical symptoms
The symptoms of dying are numerous, as are the medical conditions that cause them. Each different medical condition will dictate which symptoms are markers for the beginning of end of life.
Here are a couple:
Cancer:-
Physical decline
Weakness (Asthenia)
Weight loss
Pain
Loss of appetite
Sleep changes: drowsiness, increased or intermittent sleep, confusion when waking
Source: National Cancer Institute
Brain Tumour:-
Decreased consciousness
Difficulty swallowing (Dysphagea)
Headache
Epilepsy
Agitation and delirium
Gasping, laboured breathing with strange vocalisations and shakes or spasms (Agonal Breathing)
Source : The Brainstrust

Old Age
To die of old age is one of many misnomers we use when it comes to the human condition. We actually die as a result of complications from dysfunctional, ageing organs.
By the time we reach 70, all vital organs are ageing and some will have been doing so for 30 years or more.
The final stages, the beginning of end of life, can originate in the weakness of any one of a number of ageing organs or a failing immune system struggling to fight infection, and the symptoms be many and varied.
Old Age

To die of old age is one of many misnomers we use when it comes to the human condition. We actually die as a result of complications from dysfunctional, ageing organs.
By the time we reach 70, all vital organs are ageing and some will have been doing so for 30 years or more.
The final stages, the beginning of end of life, can originate in the weakness of any one of a number of ageing organs or a failing immune system struggling to fight infection, and the symptoms be many and varied.
This is the medical professions expectation of dying symptoms taken from a study of the old and frail including residents of a nursing home.
Anorexia and weight loss
Pain
Physical weakness (Asthenia)
Detremental changes in breathing patterns including intermittent breaks (Aponea)
Mottled skin (see image)
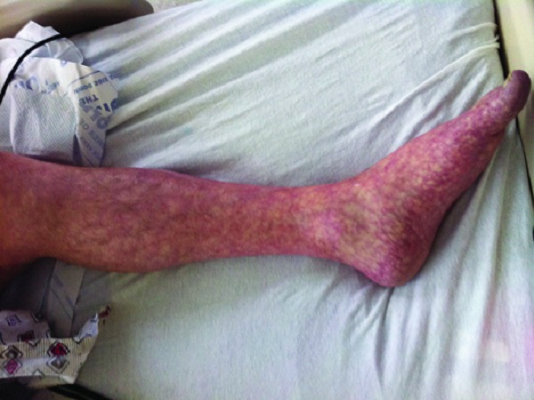
Mood changes; restlessness, anxiety and withdrawal from social interaction with residents, family and staff.
Distinctive odour. ‘The smell of death’ (rotting flesh with a dash of pineapple and raspberry, according to research).
The Hippocratic Face
This is quite literally the face of imminent death first described by Hippocrates. It happens as a result of extreme vomiting and diarrhoea, starvation or as a result of a prolonged, severe illness. Doctors view it as being as relevant today as it was when Hippocrates first documented it in ancient Greece.
Features of a Hypocratic Face:-
Sunken eyes
Sharp nose
Temples and cheeks concave
Ears cold and drawn in
Earlobes distorted
Skin hard, dry and stretched
Pale or dusky in colour
Relaxed lips

The Patients Choice
A large survey across six European countries found that, given an end of life prognosis based on a doctor’s perception of suffering, a third of cases ended in sudden death. Some of these deaths were directly attributed to drugs administered for the sole purpose of speeding up the end of life process.
On a personal note I have found myself sitting next to a drawn curtain while, on the other side hidden from view, a nurse tried to reason with a cancer patient that choosing not to live was not good option to take. It is widely accepted that a positive attitude can have positive outcomes, but people can and do choose not to prolong life.
It is true that the dying delay the end to see out an event (the birth of a child, the arrival of a relative etc). equally depression can speed the dying process with or without the prompt of a diagnosis. It’s very hard to underestimate the power of the mind when it comes to defying expectation.
DNR – Do not resuscitate order
A DNR is a legal form issued by a hospital, or at the request of the patient to withhold CPR (Cardiopulmonary Resuscitation) or life support. There are different reasons why a DNR might be issued, but broadly speaking it would be when there is a belief that there are no benefits in prolonging life, ie.
• Quality of life would suffer. CPR can cause more problems than it solves. This can include brain damage and damage to other vital organs. This would generally apply if the person is elderly or frail.
• Death has been diagnosed.
“Depression can speed the dying process”
Palliative Care
End of life Comfort and Care is the bit that happens in the last stages of Palliative Care. Both provide support and medical care to ease pain and suffering in the final stages of life, but Palliative Care also provides it in the long term. This can be in Hospital, Hospice or at home and is as much about supporting the family as the patient through medical treatments as well as the final stages of life.
If your character finds themselves in a hospice they will find the care to be softly spoken and understanding with a great deal of hand holding (metaphoric and actual). Death is not an easy concept nor a trouble free journey. There are many psychological effects, especially if the end of life prognosis is given early and allows for time to ponder on the meaning and purpose of life. The dying often look for closure; to say goodbye and forgive, or be forgiven. The care is designed to promote physical, psychological and spiritual wellbeing and includes social and care workers, spiritual professionals as well as medical staff.
A character in the last stages of end of life may not be be in pain, but they may be deeply troubled. They may act irrationally, get angry and scared, slip in and out of consciousness and delirium and see and talk to people who are already dead. Families and staff are encouraged to always act positively, speak gently (even during lapses of consciousness) and accept irrationality and hallucinations as part of a natural process.
“near death symptoms can appear at any time in the end of life process”
The End is Nigh – The final countdown to death
Yes there is a final countdown. Well, there is an expectation in Palliative Care when certain symptoms will show. In reality near death symptoms can show themselves at any time in the end of life process. Though a dying diagnosis may seem to allow a few weeks to prepare, it wouldn’t be unrealistic for your character to ‘take a turn for the worse’ and run out of time.
Dying is the process of the body shutting down. Dwindling energy reserves are stored by reducing normal functions, effectively putting your character into sleep mode. As the process progresses, the heart will stop pumping properly, blood pressure will drop and the organs, arms and legs will receive less blood. Organ function will reduce and arms and legs will bruise and swell. Oxygen levels in the blood will fall and kidney and bowel functions, especially, will reduce and produce less excretions. The urine will be darker than normal.
The Palliative Care Timeline of end of life symptoms.
One to three months.
Decreased desire for food – Food becomes less important, your character may only be able to manage small portions and begin to lose weight.
Increased desire for sleep – Not just overly tired, but also uncommunicative, unresponsive or hard to wake.
Withdrawing from people and the environment – Generally unsociable and unresponsive, detaching from normal life. Even as far as falling into a comatose type state.
One to two weeks.
Fever does happen, but it is not a given and can occur only in the very last stages
Blood pressure drops. This can cause dizziness, unsteadiness, fainting, blurred vision, palpitations, nausea and confusion.
Change is respiration – Hypopnea; Overly shallow breathing or a low respiratory rate (breaths per minute). In a healthy adult this would be 12-18 but the younger the person the higher the rate. So for a 3 year old it would be 20-30 and a 6 months 25-40. Cheyne-Stokes breathing pattern; deep and sometime faster breathing with periods of Apnea, no breathing for a few seconds to a minute. Dyspnea; Laboured or shortness of breath. Or periods of rapid shallow panting
Erratic pulse
Congestion – Gurgling sounds (sometimes loud), ‘The Death Rattle’. This is caused by secretions in the throat and the loss of the cough reflex. There is a danger of drowning if not cleared.
Incontinence
Everyone wants a good death in the final stages. In medical terms this is the usual route and means your character will become very sleepy, lethargic and drift towards a semi or fully comatose state along with the symptoms above.
A difficult route would include:-
Confusion – unable to recognise where they are or who they are with.
Restlessness – Repetitive movements including picking at bedclothes etc
Hallucinations – Speaking to people who are already died, or going to places or seeing things not visible.
The shakes
Your character may be in pain, agitated and suffer all the above, then fall into mumbling delirium. This is terminal delirium and the fear for medics is that your character will be terrified and suffer real distress. Beyond that would be to become semi-comatose and comatose, but this isn’t always the case. Your character may suffer from muscle jerks and seizures before they become semi-comatose.
Your character may have trouble swallowing (Dysphagea) and will probably stop eating and drinking and become dehydrated. It’s unlikely that the medics will do anything to restore food intake. Even in this weakened state your character will survive up to 2 weeks without food. Fluid is a different matter. Life expectancy without fluids is only 3 days, but there will be consideration as to whether using an IV could makes matters worse. The decision may be made to let nature take its course.
Days or hours.
Glassy or teary eyes
Dry, half open eyes – dehydration can cause the eyelids to shrink
Dry, slack mouth
Irregular breathing
Cyanosis – Bluish discoloration of the fingers, earlobes and nailbeds, or mucous membranes
Increased restlessness
Cold, purple, blotchy feet and hands – mottling of the skin
Weak pulse
Decreased urine output.
Minutes.
Gasping breath
Not regaining consciousness.
Death
Three final breaths
Post Mortem
Eyes open, pupils fixed
Waxy pallor
Jaw open
Muscles and the sphincter relaxed
No heartbeat
THE END
All Rights Reserved
Images Attributes
‘Between a Rock and a Hard Place’ – Fair use, https://en.wikipedia.org/w/index.php?curid=30639123
‘Old Age’ – Photo by Cristian Newman on Unsplash
‘Mottled skin’ – By Nantsupawat T et al – Nantsupawat, Teerapat (2013-01-01). “Obscure Severe Infrarenal Aortoiliac Stenosis With Severe Transient Lactic Acidosis”. Journal of Investigative Medicine High Impact Case Reports 1 (1). DOI:10.1177/2324709613479940. PMID 26425569. PMC: 4528787.</ref>, CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=55185874
‘The Hippocratic Face’ – By Rosemary A Jones – Own work, CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=50645958
References:-
Diagnosing dying: an integrative literature review –
Catriona Kennedy,1 Patricia Brooks-Young,2 Carol Brunton Gray,3
Phil Larkin,4 Michael Connolly,5 Bodil Wilde-Larsson,6 Maria Larsson,6
Tracy Smith,7 Susie Chater8. http://spcare.bmj.com/ – Published by group.bmj.com
https://www.compassionandsupport.org/index.php/for_patients_families/death_dying/signs_of_dying
//katische.com/end-of-life/the-physiology-of-death
http://dying.lovetoknow.com/Physical_Stages_of_Dying
//www.slideshare.net/KylePEdmondsMD/dying-dx-mgmt
https://www.crossroadshospice.com/caregiver-guidance/physical-emotional-changes/
https://www.theguardian.com/lifeandstyle/2015/jun/02/doctors-predict-patient-die-prognosis-wrong

