You have created a character and breathed life into them in the pages of a story. Now you need to kill them off and have chosen chronic bronchitis and emphysema, but how do you make it realistic? What is it, what happens and how? How, why and when would your character die? What changes, if any, would you need to write into your doomed character?
Read on to answer these questions and kill your character with conviction.
For more on the process of dying see ‘Killing your character convincingly – Staring Death in the Face’
What are chronic bronchitis and emphysema
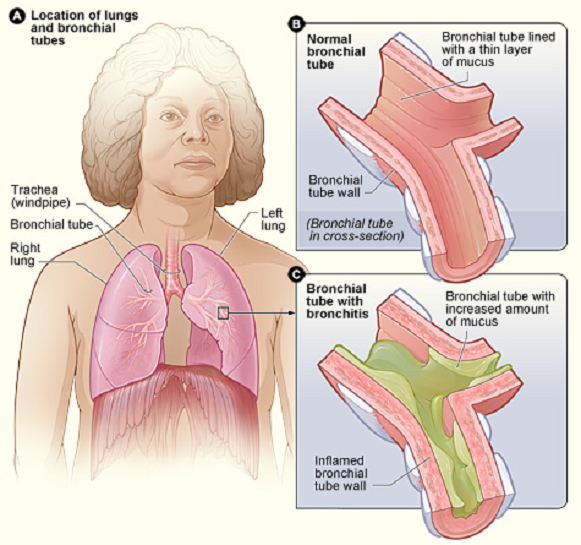
Chronic bronchitis and emphysema are both more commonly known names for COPD (Chronic Obstructive Pulmonary Disease). In technical terms bronchitis refers to the damage of the bronchial tubes and emphysema, the damage to the lungs, but they tend to come as a pair. The bronchial tubes carry air to the lungs.
The bronchi branch off on either side of your windpipe (trachea) and lead to smaller and smaller airways inside your lungs, known as bronchioles. In the lungs the air is collected in air sacs (alveoli) where carbon dioxide in the blood is exchanged for oxygen and sent out to other organs.
COPD should not be confused with acute bronchitis. Although the initial symptoms of COPD are the same as acute bronchitis, acute bronchitis is 90% airborne viral, short term and survivable with little more than hot honey drink.
Why your character dies
Blocked airways make breathing difficult and the lungs become scarred encouraging bacterial infection. Hey presto your character contracts bacterial pneumonia, develops heart failure or serious respiratory problems and dies.
In 75% of cases smoking is the cause of COPD, the other 25% are due to industrial and environmental air pollution in dust and fumes over a long period. It isn’t contagious and takes a long time to develop into a debilitating disease.
“Smoking causes 75% cases of COPD”
Your character will be over 45 and have a phlegmy cough. The cough will have been around for a year or two and happen most days of the month for three months a year. The inflamed Bronchi produce lots of mucus, the cough becomes irritating,
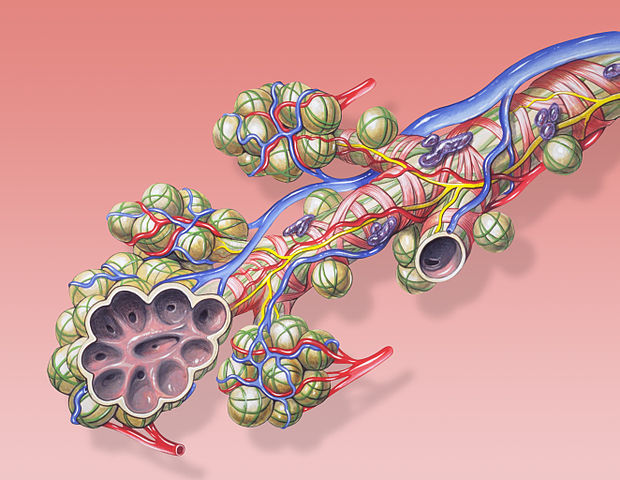
Alveoli (air sacs) in the lungs
COPD deteriorates the airways (bronchial tubes) and lungs. Over time the airways and air sacs in the lungs become slack and less efficient. The airways become thickened, irritated and inflamed, produce more mucus, become clogged and a breeding ground for bacterial infection. The walls between the air sacs are destroyed leaving larger, less efficient air sacs.
Bacterial infection in COPD is caused by the same infection that causes Influenza, Pneumonia and other respiratory infections
Symptoms:-
The main symptom is a hacking cough which may bring up clear, yellow-grey or greenish mucus (phlegm).
Other symptoms are similar to a cold, with shortness of breath and wheezing and a tight feeling in the chest.
Severe COPD can affect the most basic functions and mundane activities of living, walking or taking care of yourself, to the point where they become impossible tasks.
Medical tests include Lung function tests, chest xrays and physical examinatiions are carried out to rule out other causes. The blood is tested for oxygen levels by carrying out an Arterial blood gas test and Oximetry.
“The symptoms of COPD don’t ever really go away”
Damage to the lungs is established by testing the lungs capacity to transfer carbon monoxide. An ECG (Electrocardiogram) rules out heart disease as a cause of shortness of breath. A CT scan is sometimes used to get an overall picture of the lungs.
Treatment
The symptoms of COPD don’t go away, so the common treatments are focussed on easing the symptoms. Nebulisers and inhalers are used to ease breathing difficulties, coughs, wheezing and symptom flare ups.
More long term treatments includes breathing from a portable oxygen tank. Surgery is only considered as a last resort.
End of life symptoms include shortness of breath (Dyspnea) even when resting, lung infections, repiratory and heart failure, high resting heart rate (Tachycardia) and weight loss.
All Rights Reserved
Image Attributes:
Alveoili By helix84 – en:Image:Alveoli.jpg, CC BY 2.5, https://commons.wikimedia.org/w/index.php?curid=1737765
References:-
https://medlineplus.gov/chronicbronchitis.html
https://www.nhlbi.nih.gov/health/health-topics/topics/copd/
https://www.emedicinehealth.com/emphysema/article_em.htm
https://www.healthline.com/health/copd/end-stage-copd#copd1
https://medlineplus.gov/chronicbronchitis.html
https://www.nhlbi.nih.gov/health/health-topics/topics/copd/
https://www.emedicinehealth.com/emphysema/article_em.htm
https://www.healthline.com/health/copd/end-stage-copd#copd1